- Pendahuluan
- Patofisiologi
- Etiologi
- Epidemiologi
- Diagnosis
- Penatalaksanaan
- Prognosis
- Edukasi dan Promosi Kesehatan
- Panduan e-Prescription
Panduan e-Prescription Impetigo
Panduan e-prescription pada impetigo ini dapat digunakan Dokter pada saat akan memberikan terapi medikamentosa secara online.
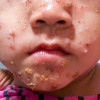
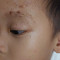
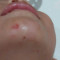
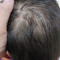
Impetigo adalah infeksi bakteri pada epidermis atau kulit superfisial. Umumnya terjadi pada anak-anak. Berdasarkan jenis lesi, impetigo terdiri dari impetigo bulosa dan nonbulosa. Kebanyakan kasus (70%) adalah impetigo krustosa atau nonbulosa, dan disebabkan oleh bakteri Streptococcus β hemolyticus. Sementara itu, impetigo bulosa disebabkan oleh Staphylococcus aureus.[1]
Tanda dan Gejala
Referensi
1. Johnson MK. Impetigo. Adv Emerg Nurs J. 2020; 42(4): 262-269
2. Perkumpulan dokter spesialis kulit dan Kelamin Indonesia (PERDOSKI). Panduan praktik klinis bagi dokter spesialis kulit dan kelamin di Indonesia. Jakarta: 2017
3. Nardi NM, Schaefer TJ. Impetigo. [Updated 2023 Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-.
4. Dollani LC. Marathe KS. Impetigo/Staphylococcal Scalded Skin Disease. Pediatr Rev. 2020; 41(4): 210-212.
5. Hassanein M, Gudsoorkar P, Padala SA, et al. Infection-Related Glomerulonephritis. [Updated 2025 Dec 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-.
6. The Royal Children Hospital Melbourne. Impetigo (school sores). 2025. https://www.rch.org.au/kidsinfo/fact_sheets/Impetigo_school_sores/
7. May PJ, Tong SYC, Steer AC. et al. Treatment, prevention and public health management of impetigo, scabies, crusted scabies and fungal skin infections in endemic populations: a systematic review. Trop Med Int Health. 2019; 24(3): 280–293.
8. American Academy of Dermatology Association. Impetigo: Diagnosis and treatment. 2021. https://www.aad.org/public/diseases/a-z/impetigo-treatment .
9. Francis SF, Sasirekha B, Prabhu R, et al. Impetigo – A case report. IJRRJournal. 2018; 5(11): 12-14.
10. Schachner LA, Andriessen A, Benjamin LT, et al. Do Antimicrobial Resistance Patterns Matter? An Algorithm for the Treatment of Patients With Impetigo. J Drugs Dermatol.2021; 20(2); 134-142.
11. Van Ravenstein K, Williams TH. Diagnosis and management of impetigo. Nurse Pract. 2017; 42(3): 41-44.
12. Clebak KT, Malone MA. Skin Infections. Prim Care. 2018;45(3):433-454.
13. Hartman-Adam H, Bancvard C, Juckett G. Impetigo: Diagnosis and Treatment. Am Fam Physician. 2014; 90(4): 229-235.
14. MIMS Indonesia. Amoxicillin + Clavulanic acid. 2026. https://www.mims.com/indonesia/drug/info/amoxicillin%20+%20clavulanic%20acid?mtype=generic
15. MIMS Indonesia. Cefalexin. 2026. https://www.mims.com/indonesia/drug/info/cefalexin?mtype=generic
16. MIMS Indonesia. Dicloxacillin. 2026. https://www.mims.com/indonesia/drug/info/dicloxacillin?mtype=generic
17. MIMS Indonesia. Cefadroxil. 2026. https://www.mims.com/indonesia/drug/info/cefadroxil?mtype=generic
18. MIMS Indonesia. Vancomycin. 2026. https://www.mims.com/indonesia/drug/info/vancomycin?mtype=generic
19. MIMS Indonesia. Clindamycin. 2026. https://www.mims.com/indonesia/drug/info/clindamycin?mtype=generic
20. MIMS Indonesia. Doxycycline. 2026. https://www.mims.com/indonesia/drug/info/doxycycline?mtype=generic
21. Moon AT. Impetigo Medication. 2025. https://emedicine.medscape.com/article/965254-medication#4
22. MIMS Indonesia. Cetirizine. 2026. https://www.mims.com/indonesia/drug/info/cetirizine?mtype=generic
23. MIMS Indonesia. Loratadine. 2026. https://www.mims.com/indonesia/drug/info/loratadine?mtype=generic
24. Malka, Ziy M. Safety of Common Medications for Treating Dermatology Disorders in Pregnant Women. Curr Dermatol rep. 2013; 2: 249-257.
25. Drugs.com. Retapamulin topical Pregnancy Warnings. 2026. https://www.drugs.com/pregnancy/retapamulin-topical.html
26. Drugs.com. Ozenoxacin topical Pregnancy Warnings, 2025. https://www.drugs.com/pregnancy/ozenoxacin-topical.html
27. Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: update by the infectious diseases society of America. Clin Infect Dis. 2014;59(2):147.
28. Williamson DA, Monecke S, Heffernan H, et al. High usage of topical fusidic acid and rapid clonal expansion of fusidic acid-resistant Staphylococcus aureus: a cautionary tale. Clin Infect Dis. 2014;59(10):1451.
(Konten ini khusus untuk dokter. Registrasi untuk baca selengkapnya)