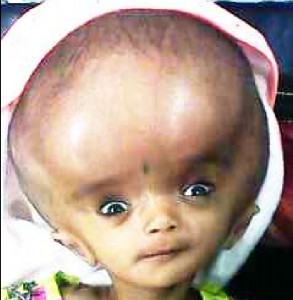
Diagnosis Hydrocephalus
Diagnosis hydrocephalus kongenital pada neonatus, bayi, dan anak-anak, adalah berdasarkan lingkar kepala (occipito-frontal) yang besar saat lahir, ataupun pemeriksaan lingkar kepala serial yang menunjukkan peningkatan yang lebih dari sebagaimana mestinya.
Sedangkan hydrocephalus yang didapat (acquired) biasanya datang dengan gejala-gejala yang berhubungan dengan peningkatan tekanan intrakranial (TIK), seperti nyeri kepala, gangguan penglihatan, mual muntah, bahkan penurunan kesadaran. Pemeriksaan untuk konfirmasi adalah pencitraan otak, baik dengan CT scan kepala, maupun MRI otak. Untuk mengukur tekanan intrakranial, perlu dilakukan test pressure opening pada pungsi lumbal, dengan posisi lateral dekubitus.[1,35,36,51]
Anamnesis
Anamnesis pada hydrocephalus dibagi berdasarkan onsetnya, yaitu kongenital atau didapat (acquired) pada pasien anak dan dewasa. Pada anak-anak dan dewasa tanda peningkatan TIK seperti nyeri kepala, gangguan penglihatan, dan gait disturbance.
Hydrocephalus Kongenital
Anamnesis untuk hydrocephalus kongenital seringkali didapatkan secara alloanamnesis dari orang tua sejak antenatal, saat pemeriksaan ultrasonografi (USG) kepala janin. Pada bayi, kecurigaan hydrocephalus kongenital dari anamnesis biasanya didapat dari orang tua berdasarkan riwayat kunjungan antenatal.
Anamnesis pada hydrocephalus kongenital harus dapat menggali kemungkinan etiologi dan faktor risiko, seperti riwayat keluarga dengan keluhan yang sama, infeksi dan penyakit saat kehamilan, kunjungan antenatal, usia janin saat dilahirkan, serta penggunaan obat-obatan dan alkohol.[13,15-19]
Hydrocephalus tipe Acquired pada Anak
Pada anak, hydrocephalus tipe acquired biasanya datang dengan keluhan nyeri kepala, gangguan penglihatan (blur atau spotty), penurunan kesadaran, serta mual dan muntah, karena adanya peningkatan TIK. Anamnesis harus ditanyakan kepada orang tua adalah riwayat antenatal serta persalinan anak, serta riwayat tumor otak dan cedera kepala. Selain itu, perlu ditanyakan riwayat tumbuh kembang anak, termasuk adanya gangguan kognitif dan prestasi akademik.[1,37,52]
Hydrocephalus tipe Acquired pada Orang Dewasa
Pada anamnesis hydrocephalus tipe acquired pada orang dewasa juga ditemukan gejala-gejala yang disebabkan peningkatan TIK, yang bersifat akut maupun kronis. Pada normal pressure hydrocephalus (NPH), dapat ditanyakan keluhan trias Hakim, yaitu kesulitan untuk menahan BAK (inkontinensia urine), keluhan gangguan kontrol mobilitas, dan gangguan kognitif/retardasi mental.
Selain itu, pada orang dewasa perlu ditanyakan mengenai etiologi dan faktor risiko, termasuk riwayat gangguan vaskular, seperti hipertensi, diabetes mellitus, dan dislipidemia, serta riwayat stroke.[10,12,25-29,52]
Pemeriksaan Fisik
Pemeriksaan fisik pada hydrocephalus tidak lepas dari manifestasi klinis yang terjadi karena adanya peningkatan TIK dan dilatasi ventrikel. Manifestasi klinis bervariasi berdasarkan usia.
Neonatus
Pada neonatus, manifestasi klasiknya adalah apnea dan bradikardi serta ukuran lingkar kepala (occipito-frontal) yang lebih besar daripada normal. Penilaian ukuran lingkar kepala dilakukan dengan plotting pada kurva lingkar kepala untuk usia 0-2 tahun, serta tanda klinis sutura kranialis yang terlihat melebar.
Manifestasi apnea dan bradikardi ini berdasarkan trias Cushing yang terjadi pada keadaan terjadinya peningkatan tekanan intrakranial, yaitu hipertensi, bradikardi dan pola pernapasan yang ireguler.[1,38]
Bayi
Manifestasi klinis yang khas pada bayi adalah ukuran kepala di atas 2 SD sesuai usia atau makrosefali. Pada kelompok usia ini, manifestasi apnea dan bradikardi sudah tidak terlalu terlihat. Perubahan perilaku dan penurunan kesadaran (letargi dan iritabilitas) dapat diamati dengan jelas pada kelompok usia ini. Muntah-muntah dan penurunan berat badan juga dapat terjadi.[1,39]
Manifestasi klinis yang khas pada neonatus dan bayi antara lain, kepala yang mengalami pembesaran yang lebih dari normal, baik ukuran maupun kecepatan pembesarannya, bulging pada fontanel anterior, sering mengantuk, irritable, kejang, sunsetting of the eyes, serta gangguan perkembangan.[1,38,39]
Gambar 3. Hydrocephalus dengan Sunsetting of the Eye. Sumber: شہاب, Wikimedia Commons, 2017
Sunsetting of the eye disebabkan karena adanya tekanan pada midbrain sehingga menyebabkan gangguan pergerakan bola mata saat melirik ke atas. Sunsetting of the eye yang dimaksud adalah terlihatnya sklera di atas iris. Adanya peningkatan tekanan intrakranial juga dapat memberikan manifestasi papilledema pada pemeriksaan funduskopi.[1,38,39]
Anak-anak
Pada anak-anak, fontanel dan sutura sudah menutup dan kemampuan kompensasi kranium menurun, sehingga gejala akut lebih mudah terlihat pada kelompok usia ini. Anak dapat terlihat letargi dan irritable, dengan gangguan neurologis fokal seperti kelemahan saraf kranial VI bilateral, yaitu tidak mampu mengabduksi kedua mata dan diplopia. Diplopia juga disebabkan oleh adanya penekanan pada otot ekstraokular. Perkusi area kepala pada bagian ventrikel yang dilatasi didapatkan suara panci pecah atau crackpot sound (Macewen's sign).[1,37]
Manifestasi klinis yang menunjukkan adanya late-stage hydrocephalus dan mengindikasikan perlunya intervensi segera adalah kejang onset baru dan sindrom Parinaud (dorsal midbrain syndrome). Sindrom Parinaud terdiri dari gejala khas kelumpuhan upgaze, yaitu pupil mampu berakomodasi tapi tidak mampu bereaksi terhadap cahaya (pupil pseudo-Argyll Robertson), nistagmus konvergen, dan Collier sign (retraksi abnormal palpebra).[1]
Dewasa
Pemeriksaan fisik hydrocephalus pada orang dewasa, seperti pada pasien anak-anak, dapat ditemukan:
- Papilledema, karena pembengkakan saraf optik
- Keterbatasan pandangan ke atas, karena tekanan pada lempeng tektal melalui reses suprapineal
- Cara berjalan (gait) yang limbung/unsteady
- Ukuran kepala relatif besar
- Kelumpuhan saraf keenam unilateral atau bilateral[1,42]
Pada normal pressure hydrocephalus (NPH) ditemukan trias gejala klasik, yaitu gangguan kognitif (demensia), gangguan gaya berjalan (apraxia), dan inkontinensia urine. Demensia dapat dinilai dengan melakukan pemeriksaan mini mental state examination (MMSE).
Apraxia dapat dinilai dari cara berjalan pasien dan gejala upper motor neuron, seperti hiperrefleks, spastisitas, klonus pada ekstremitas inferior, serta refleks Babinski positif yang disebabkan karena adanya stretching dan gangguan pada serat kortikospinal untuk regio extremitas bawah pada korteks motorik. Gejala ini biasanya bilateral dan simetris, sehingga apabila terdapat lateralisasi, kemungkinan diagnosis ke arah NPH dapat disingkirkan.[5,10,11,40]
Diagnosis Banding
Diagnosis banding untuk hydrocephalus meliputi penyakit yang berhubungan dengan peningkatan tekanan intrakranial (TIK) dan dilatasi ventrikel.
Hipertensi Intrakranial Idiopatik (HII)
Hipertensi intrakranial idiopatik (HII) adalah peningkatan tekanan intrakranial yang tidak disertai dengan kelainan patologis pada morfologi intrakranial, yang dapat dilihat dengan pencitraan. Hipertensi intrakranial idiopatik (HII) seringkali ditemukan pada perempuan usia produktif dengan gejala klinis berupa nyeri kepala, gangguan penglihatan/gangguan lapang pandang, pulsatile tinnitus, dan nyeri pada leher.
Diagnosis ditegakkan dengan memenuhi kriteria Dandy dan CT scan kepala atau MRI otak, namun MRI lebih dipilih. Pemeriksaan MRI otak akan menunjukkan penipisan kelenjar hipofisis (empty sella sign), dilatasi ruang ventrikel di sekitar saraf optikus, penipisan lingkar bola mata bagian dorsal, papila yang prominen pada saraf optikus, serta stenosis sinus transversa.[41]
Atrofi Otak Terkait Usia
Seiring dengan bertambahnya usia, terjadi penurunan volume otak fisiologis. Berbeda dengan hydrocephalus, perubahan ini menimbulkan dilatasi ruang ventrikel secara simetris. Atrofi otak terkait usia ini terutama mengenai korteks sensorimotor, korteks visual dan oksipital, frontal dan thalamus.
Hal ini berbeda dengan atrofi otak patologis, seperti pada demensia. Dilatasi ventrikel pada atrofi otak patologis biasanya non-spesifik, beberapa tipe dapat memberikan konklusi berupa penyakit utamanya, misalnya atrofi hipokampus pada demensia Alzheimer.[41]
Atrofi Sekunder
Atrofi sekunder ini biasanya terjadi pada penyakit autoimun, HIV, post-kemoterapi, penyakit neurodegeneratif, atau setelah mengkonsumsi obat tertentu. Dehidrasi juga dapat menyebabkan dilatasi ventrikel temporer. Dilatasi ventrikel dapat terjadi simetris baik pada ruang internal dan eksternal. Keadaan ini dapat dibedakan dengan penyakit lainnya dengan menghubungkan hasil pencitraan, gejala, serta anamnesa.[41]
Pemeriksaan Penunjang
Pemeriksaan penunjang untuk menunjang diagnosis hydrocephalus meliputi pencitraan, (ultrasonografi, CT scan, MRI) dengan menemukan pelebaran ruang ventrikel, pungsi lumbal, dan pemeriksaan laboratorium.
Ultrasonografi (USG) dan MRI Antenatal
Ultrasonografi antenatal adalah pencitraan hydrocephalus yang pertama kali dapat dilakukan, dimana pada kepala fetus terlihat adanya pelebaran ventrikel, normalnya adalah <10mm. Pada USG pasien hydrocephalus ditemukan “butterfly” sign pada plexus koroid ventrikel lateral potongan transversal. Hydrocephalus biasanya sudah dapat terdeteksi pada saat memasuki kehamilan trimester kedua kemudian dapat dikonfirmasi dengan fetal MRI untuk melihat gambaran otak secara detail.[46,47]
Pemeriksaan MRI fetus berguna untuk mengidentifikasi struktur ventrikel dan melakukan volumetri ventrikel. Pemeriksaan MRI digunakan untuk mengevaluasi ventrikulomegali, karena modalitas ini dapat mengidentifikasi abnormalitas tertentu yang tidak dapat dideteksi dengan USG, misalnya malformasi kortikal dan migrasi yang abnormal. Pemeriksaan MRI paling baik digunakan pada usia kehamilan 22–24 minggu, karena saat ini adalah puncak perkembangan sistem saraf pusat.[48,49]
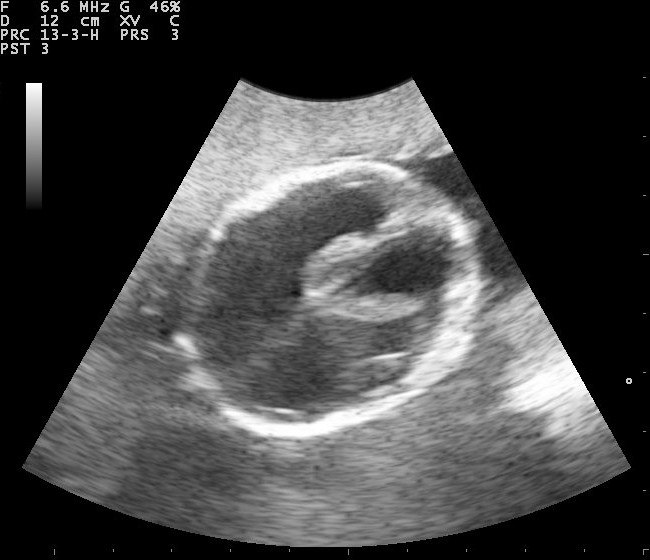 Gambar 4. Gambaran Ultrasonografi pada Fetus dengan Hydrocephalus. Sumber: Nevit Dilmen, Wikimedia commons, 2010
Gambar 4. Gambaran Ultrasonografi pada Fetus dengan Hydrocephalus. Sumber: Nevit Dilmen, Wikimedia commons, 2010 Ultrasonografi (USG) Kepala Bayi
Bayi yang dicurigai hydrocephalus dapat dilakukan skrining dengan USG (point-of-care ultrasonography/POCUS) untuk identifikasi dan monitoring, terutama pada keadaan gawat darurat. Teknik yang digunakan adalah transfontanela POCUS, dengan transduser 5-10 MHz. Probe diletakkan pada fontanel anterior, yang masih terbuka sampai usia 2 tahun, tetapi pemeriksaan ini akan memberikan gambaran yang lebih maksimal pada usia 12–18 bulan dimana fontanel anterior masih paten. Pemeriksaan ini kemudian dapat memvisualisasi sistem ventrikel yang dilatasi.[39]
Tanda awal hydrocephalus yang dapat terlihat adalah pelebaran atau “ballooning” kornu anterior ventrikel lateral. Selanjutnya akan terjadi dilatasi konsentrik dan memperlihatkan pembesaran kornu frontalis membentuk lingkaran menyerupai telinga “Mickey Mouse”. Indeks bifrontal adalah rasio bagian kornu anterior yang terluas dibandingkan dengan bagian terluas dari bagian dalam kranium (normalnya 0,3), apabila >0,5 maka dapat dicurigai hydrocephalus.[39]
CT Scan Kepala dan MRI Otak
Diagnosis hydrocephalus dapat ditegakkan dengan melakukan pemeriksaan neuroimaging, antara lain seperti CT scan kepala, atau MRI otak. Pemeriksaan neuroimaging ini juga dapat membantu mengetahui adanya malformasi maupun tumor. Selain itu juga dapat mengetahui bagian yang mengalami obstruksi, dengan melihat adanya dilatasi ventrikel pada bagian tersebut.
Pemeriksaan CT scan sebenarnya sudah sensitif untuk mendiagnosis NPH dan adanya ventrikulomegali, namun MRI dapat memberikan informasi tambahan yang penting, misalnya adanya stenosis aqueductus, perubahan substansia alba (hipersensitivitas substansia alba), maupun adanya etiologi lain (seperti demensia Alzheimer).[11]
Pemeriksaan CT scan kepala dapat membantu untuk menilai ukuran ventrikel dan struktur lain di otak. Kriteria hydrocephalus akut CT scan antara lain, pembesaran kornu temporal bilateral lebih dari 2mm yang jelas terlihat, dalam keadaan normal kornu temporalis hampir tak terlihat.
Gambar 5. Gambaran MRI pada Hydrocephalus dengan Mickey Mouse Sign. Sumber: Nevit Dilmen, Wikimedia Commons, 2005
Rasio bagian terlebar kornu frontalis dengan diameter biparietal yang maksimal (Evans ratio) lebih dari 30%. Adanya ballooning pada kornu frontalis ventrikel lateral dan ventrikel ketiga (mickey mouse sign) dapat juga mengindikasikan adanya obstruksi aquaductus. Selain untuk keperluan diagnosis, CT scan juga dapat digunakan untuk memonitor pasien dengan hydrocephalus post-shunting.[11,31]
Pemeriksaan MRI otak dapat dengan kontras dapat melihat kuantitas aliran cairan serebrospinal pada aquaductus dan memprediksi angka responsivitas shunt. Selain itu, metode ini juga dapat mengukur tekanan intrakranial secara tidak langsung, sehingga mengurangi keperluan tindakan invasif. [45]
Positron Emission Tomography (PET)/Single Photon Emission Tomography (SPECT) Cerebral Blood Flow dan Brain Metabolic Studies
Pemeriksaan positron emission tomography (PET)/single photon emission tomography (SPECT) pada aliran pembuluh darah otak dan status metaboliknya dapat dievaluasi 1 minggu sebelum dan 7 bulan setelah dilakukan tindakan operasi pada pasien dengan normal pressure hydrocephalus (NPH).
Adanya perbaikan setelah terapi shunting digambarkan dengan menurunnya aliran darah otak. Adanya perbaikan kemampuan metabolik ini menandakan perbaikan neurologis, yang berarti ada perbaikan hemodinamik. Adanya hipometabolik pada area korteks menunjukkan menurunnya penggunaan glukosa.[36,45]
Pemeriksaan Pungsi Lumbal
Pemeriksaan pungsi lumbal dilakukan apabila dicurigai adanya etiologi infeksi, misalnya yang menyebabkan adhesive arachnoiditis atau ependimitis. Selain itu, pemeriksaan pungsi lumbal atau tap test, dapat digunakan untuk menunjang diagnosis normal pressure hydrocephalus (NPH), dengan mengaspirasi 40-50 ml cairan serebrospinal (tap test) dan didapatkan perbaikan gejala klinis.
Penilaian opening pressure saat pungsi lumbal pada NPH perlu dilakukan, karena nilainya akan normal (10-20 cmH2O). Kontraindikasi tindakan ini adalah pasien dengan bukti adanya space occupying lesion (SOL), karena hal ini berisiko menyebabkan herniasi serebral. Selain itu, tap test juga tidak boleh dilakukan pada pasien dengan peningkatan tekanan intrakranial, yaitu pasien dengan tanda papilledema, defisit neurologis fokal, dan penurunan kesadaran.[11,43,44]
Pemeriksaan cairan serebrospinal yang didapatkan pada pungsi lumbal untuk menilai biomarker untuk NPH, antara lain tumor necrosis factor (TNF) alfa, amyloid-beta, laktat, protein Tau, dan triple protein neurofilamen. Biomarker ini dapat membantu memprediksi outcome kognitif pasien, mengetahui adanya mekanisme yang mendasari gangguan perkembangan, dan melakukan analisis genetik. Akan tetapi, penggunaannya dalam praktik klinis sehari-hari masih jarang dilakukan mengingat biaya dan ketersediaan sarana.[45]
Pemeriksaan Laboratorium
Tidak ada pemeriksaan darah spesifik yang direkomendasikan sebagai pemeriksaan penunjang untuk menegakkan diagnosis hydrocephalus. Pemeriksaan laboratorium yang dapat dilakukan antara lain adalah pemeriksaan genetik untuk mengetahui etiologi maupun faktor risiko yang berhubungan dengan kelainan maupun mutasi genetik.[17,42]
Direvisi oleh: dr. Felicia Sutarli